An obstetrician failed to treat a pregnant woman's dangerously high blood pressure before she suffered a stroke and died at Calvary Hospital, a coroner has found.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The ACT Coroner's Court delivered its findings on the case of Corrina Medway, 32, who died of a "massive" cerebral haemorrhage after giving birth to two girls at Calvary Hospital in May 2011.
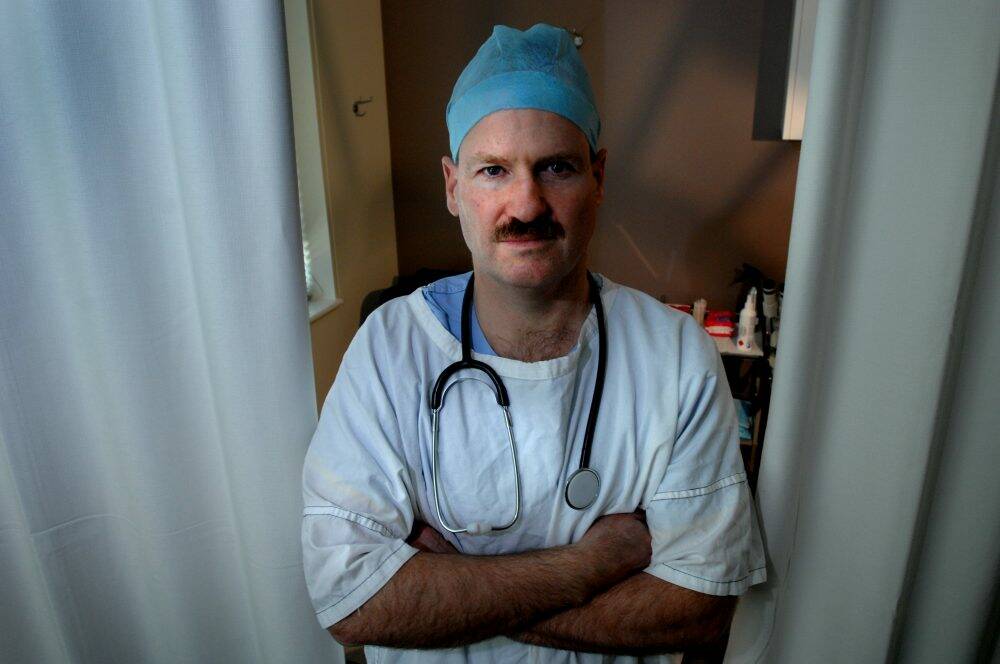
Mrs Medway's death was caused by pregnancy-induced hypertension, or abnormally high blood pressure.
Obstetrician Dr Andrew Foote was strongly criticised for his treatment of Mrs Medway in damning findings handed down by Coroner Margaret Hunter on Friday afternoon.
She found he knew of her dangerous blood pressure readings at 6pm on the night before her death, but failed to administer appropriate treatment.
That treatment, she said, was readily available in the form of rapidly acting anti-hypertension drugs.
"It is my view, and I am satisfied to the requisite standard, that Dr Foote failed to administer appropriate treatment for the acute pregnancy-induced hypertension suffered by Ms Medway between 18:00 to 18:30 hours," Ms Hunter found.
"Dr Foote's failure to treat Ms Medway's acute pregnancy induced hypertension ... resulted in her blood pressure continuing to escalate to a critical level which ultimately caused her cerebral haemorrhage and death.
"Further, I am satisfied that treatment was available within a reasonable period of time sufficient to have ameliorated the significantly high blood pressure."
Ms Hunter recommended that all nursing staff, midwives, general medical practitioners, and specialist obstetricians undergo specific training on pregnancy-induced hypertension and that literature on pre-eclampsia be provided to pregnant women under their care.
Mrs Medway first noticed something was wrong on May 13, six days before the birth of her twins, when she went to Yass Hospital complaining of swelling in her feet and hands, and pins and needles in her arms.
Elevated blood pressure was recorded, and Dr Foote put her on the drug Labetalol, a beta-blocker used to treat hypertension.
She continued to experience swollen feet and tingling sensations in her hands.
Three days later, Mrs Medway was admitted to Calvary Private Hospital, and Dr Foote advised staff to withhold and later cease the Labetalol altogether.
On May 19, the day of the twins' birth, she began to experience pain that she did not believe to be associated with contractions. Her blood pressure began to increase, and she had pain in back and shoulder tips, prompting Dr Foote to order Panadeine Forte, an epidural and later morphine. He believed the pain was muscoskeletal.
She gave birth to the twins about 3pm, but her blood pressure skyrocketed five hours later.
Midwives at the hospital gave evidence that Dr Foote knew of the high readings. Despite that, no medications were given to lower the blood pressure.
A leading expert on perinatal medicine, Professor Shaun Brennecke, gave evidence to the inquest that there were a range of readily available medicines that would have acted quickly, including hydralazine, labetalol, and nifedipine.
Professor Brennecke said there would have been no downside to giving Mrs Medway labetalol.
Dr Foote left the hospital and asked to be updated.
Mrs Medway's condition deteriorated significantly and she was rushed to the Canberra Hospital for neurosurgery. She died on May 22.
The Medical Board of Australia's professional standards hearing into the death found the allegation that Dr Foote failed to correctly diagnose the hypertensive disorder was not proven.
It accepted there was conflicting evidence in the case and that the postnatal hypertension did not warrant immediate intervention.
In his evidence to the inquest, Dr Foote claimed he had not been told of a drastically elevated blood pressure reading, which he described as a "game changer".
Had he known, he said he would have done something about it.
Dr Foote also claimed he did not want to give her anti-hypertensives without a diagnosis.
Ms Hunter rejected that evidence, and she described Dr Foote as "not entirely forthcoming" in his evidence.
"I also noted that he tended to blame others for what was basically his responsibility," she said.
"At times I was of the view that Dr Foote was not being entirely truthful."

