The medical miracles that today's hospitals can deliver for patients with life-threatening illnesses and injuries often exact a huge price. There are the known and expected financial costs, but there are also long-term, often life-altering, physical, cognitive and mental impairments for the patients who survive their acute episode.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
These are more likely the longer a patient is in hospital and most commonly associated with intensive care episodes, especially for patients who undergo mechanical ventilation. They are under-recognised and under-diagnosed, leaving patients, their families and often their doctors struggling to understand and address the issues that subsequently arise.
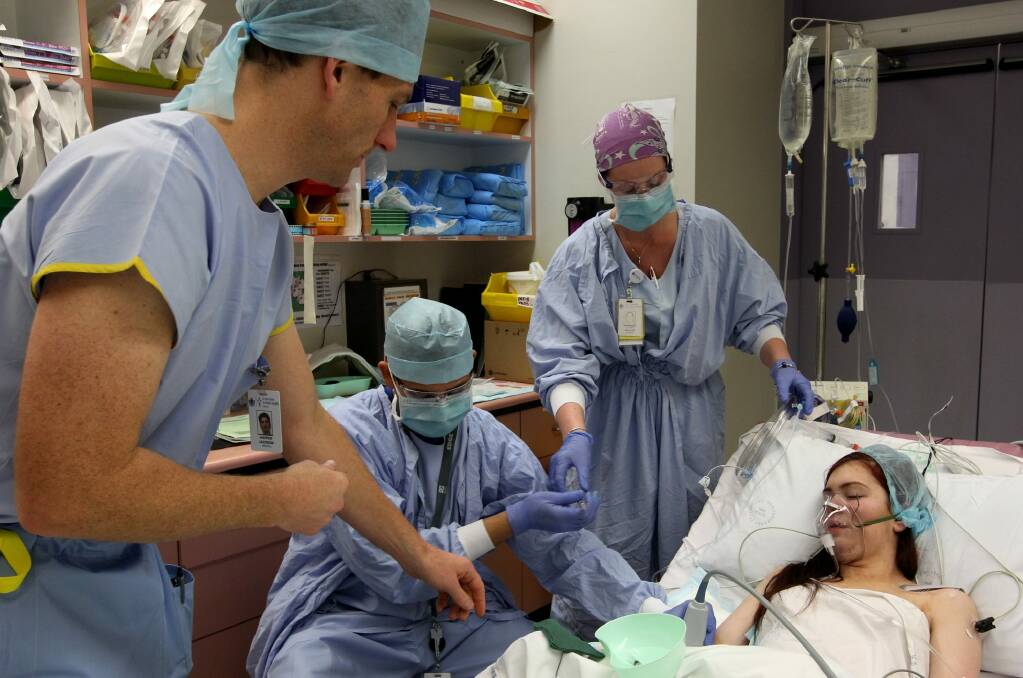
Extended hospitalisation can lead to significant deterioration of physical and mental functions, especially in the elderly, but even in children. In Australia some 150,000 patients (adults and children) are admitted to Intensive Care Units every year and most of these patients (some 75 per cent) are discharged home. Many more patients have significant hospital stays. For such patients, their successful recovery needs to focus on more than the illness or injury that precipitated their hospitalisation.
Lying in bed and immobilisation can have considerable effects on nearly every organ system in the body and it is estimated that there is a 10 per cent loss in muscle strength for every week of bed rest. This can mean the difference between dependence and independence for an older patient and slow rehabilitation for younger patients.
Efforts are routinely made to get and keep patients mobile, but these rely on busy nursing staff and allied health professionals having time to do this. One study estimated that the average hospital patients walks for only 43 minutes a day.
On discharge, patients are also often sleep deprived, poorly nourished, in pain and discomfort, and facing stressful and mentally challenging situations. Patients who have been in intensive care face a profusion of problems, including impaired pulmonary function, difficulty swallowing and mental health disorders that can mimic post-traumatic stress syndrome.
Patients need referral services and medical follow-up for these problems as well as for the condition that first brought them to hospital. Malnutrition can affect recovery and wound healing and reduced stamina and co-ordination increases the risk of falls and makes it harder to resume activities of daily living.
One problem that too often goes unnoticed and untreated is hospital-acquired delirium. This is a common and dangerous condition which typically lasts anywhere from a couple of days to several weeks but can even last months. It is caused by a combination of numerous factors, including surgery, infection, isolation, dehydration, poor nutrition and medications such as painkillers, sedatives and sleeping pills. Up to a third of patients aged 70 and over experience delirium and the rate is much higher for those in intensive care or undergoing surgery.
However, it can be prevented and treated. Some of the modifying factors include less noise, not waking sleeping patients unnecessarily, windows and clocks in patients' rooms, and making sure patients have access to their hearing aids and eyeglasses. Early psychological intervention is also important.
Failure to understand and address the impact of what is loosely termed "hospital-associated dysfunction" is costly for the healthcare system and for patients. It can lead to longer hospital stays, re-admittance in the period immediately after discharge, and failure to follow medical advice and make follow-up medical appointments. Older people may be wrongly diagnosed with dementia and lose their independence.
Clearly what is needed is more research and initiatives on how to make hospitalisation less toxic. We should not be so consumed with technological and surgical wonders that we miss their adverse impacts on the very patients whose lives they save.
The National Health and Hospitals Reform Commission report has some recommendations that could begin this effort. It proposed increased investment in and expansion of sub-acute services, and more efficient and effective transfers of patients' care to these and other, non-hospital settings. In some case this might mean initiatives such as hospital-in-the-home to keep patients out of hospital completely.
These approaches should not permit the 'quicker and sicker' discharge of patients or the substitution of alternatives to hospital care solely on the basis of cost. Rather they should be patient-centred and patient outcome-driven. Such initiatives will require new resources (the cost of which will be at least partially offset over the medium to long term by savings), improved links with community-based health and social services, and changes in culture from governments, bureaucrats, clinicians and patients.
Dr Lesley Russell is adjunct associate professor at the Menzies Centre for Health Policy at the University of Sydney.

