It was an increasingly prickly Andrew Barr who fended off questions this week.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The Chief Minister, under fire for not releasing a detailed roadmap out of lockdown, finally snapped on Thursday.
"I've been criticised and we've got a couple of journalists here running that line. But maybe I just have a higher value on human life and protecting people. I'll plead guilty to that," he said.
His frustrated chief health officer, Dr Kerryn Coleman, said Delta was rendering seemingly solid plans redundant within days.
"If we went out last week or the week before with some very solid dates ... I suspect that about half of that would need to change," she said on Friday.
While NSW and Victoria have both pencilled in timelines for schools reopening, with significant caveats, Canberra parents remain in the dark for now.
And the prospect of their children returning to the classroom while groups of students remain unvaccinated has raised concerns for some.
Data from the UK explains where some of the concern originates. On September 16, more than 1 per cent of the country's schoolchildren missed a day due to a suspected or confirmed COVID-19 case.
MORE COVID-19 NEWS:
The country abruptly lifted all restrictions in mid-July, and every school is set to reopen by the end of the month.
But with the virus highly unlikely to lead to severe symptoms in children, experts in Australia insist safely reintegrating them into the classroom is possible.
ANU infectious diseases physician Peter Collignon says children, like all adults, are more likely to contract the Delta strain than previous variants.
But he is upbeat about the coming months, with current evidence suggesting the new strain does not produce more severe symptoms.
"I think we've got to be very careful about not being pessimistic about what's going to happen to children over our upcoming summer," he says.
"The modelling says this could be really bad, but a lot of the modelling in the past has been quite off with its calculations and predictions."

Professor Collignon is urging Australians to focus on real-life data, rather than projections, saying the experience of the UK provides hope over Delta's impact on the young.
He says in Britain, where Delta has been the predominant strain for months, roughly five children are admitted to hospital out of every 100,000.
Of those, only one-fifth progress to intensive care.
"That actually means, worst-case scenario, we might have three or four admissions per week [in the ACT]," he says.
"Most of those children get well pretty quickly, some may stay for longer ... But deaths are very uncommon."
The UK's abrupt reopening, dubbed "Freedom Day", was markedly different to the staggered reopening planned across Australia.
And Professor Collignon says Canberra's fortunes are bolstered by better weather over summer, more open space than many parts of the UK, and more effective housing.
"England is a worst-case scenario. And even if you look at the worst-case scenario, it's not going to overwhelm our system," he says.
"Real-world data says, over summer at least, we shouldn't expect to have huge numbers of children admitted to hospital.
"I think we will do better than England has done."
Students aged 12 to 15 in England and Scotland are being offered a single Pfizer dose, in a move the government hopes will avoid major disruption.
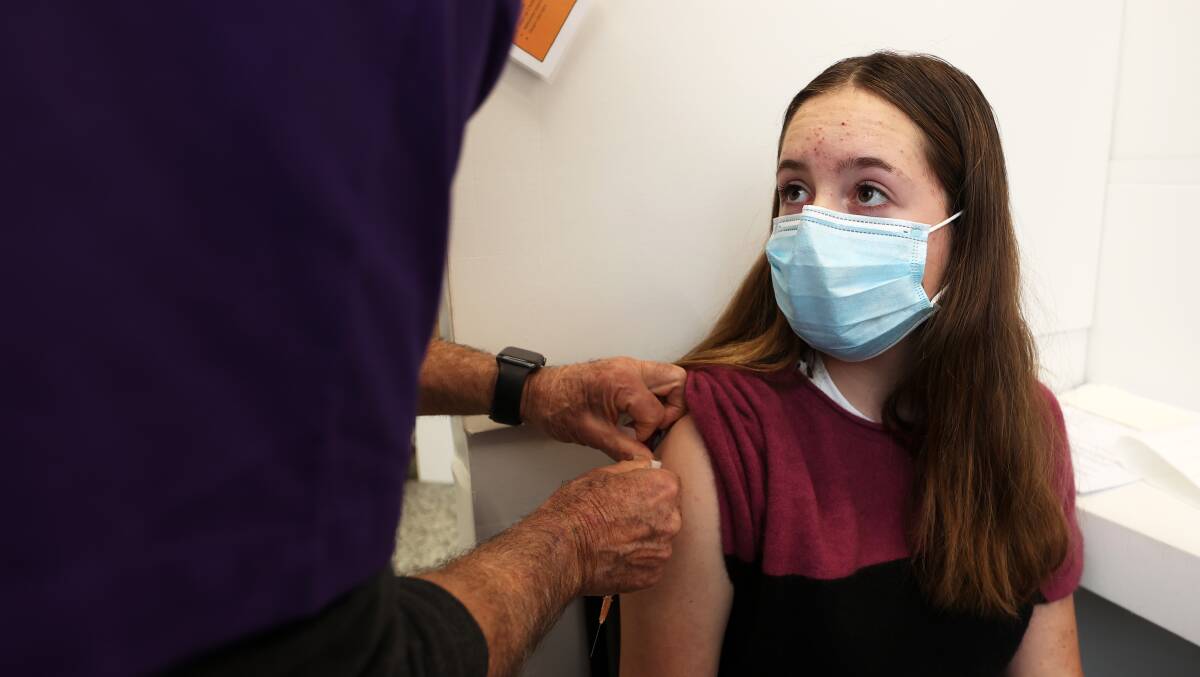
In the ACT, 3900 of 12- to 15-year-olds (19.8 per cent) have received at least one dose, while 397 (2 per cent) are fully vaccinated. It comes just six weeks after Pfizer began rolling out to the cohort, beginning with Indigenous and immunocompromised children.
And Pfizer this week declared its vaccine is safe and effective in five- to 11-year-olds, and is seeking authorisation from regulators in the US. The revelation followed a trial among 2200 children, though the company did not share efficacy data.
Pfizer says the study shows a smaller dose, 10 milligrams compared to the 30 milligrams given to people aged over 12, is enough to trigger an immune response in young children.
But Professor Collignon warns the declaration, which immediately gained global media coverage, implied too much given the "very preliminary" data set.
He stresses issues with the AstraZeneca vaccine, linked to an extremely rare blood-clotting disorder, did not emerge until it was rolled out to a large number of people.
"There are lots of things we have to know before we roll this out. They are almost implying that ... tens of millions of children can be vaccinated," he says.
"I think that is very misleading and, in my view, unethical as they presented the data.
"You should not have these announcements as a press release from the company that's going to make a lot of money."
MORE COVID-19 NEWS:
Professor Collignon says the question of whether young children, who are at significantly less risk from the virus, should be vaccinated should solely hinge on the benefit vaccines provide to them. Using them as a means to reach herd immunity, which took years to reach with disease like measles, is unrealistic, he says.
"It's not going to happen. That's why it's essential we only vaccinate children when we can clearly show the benefits to children far outweigh any downside," he says.
Infectious diseases paediatrician Robert Booy says the questions over child vaccination need to be "very carefully discussed".
He says there is "no urgent rush" to vaccinate under-12s, and Australia has the benefit of waiting to see what happens elsewhere.
"We can get primary school kids back to school without a vaccine in their arm," he says.
"We have to be completely reassured from large surveillance in the US that there aren't rare side effects that are worrying."
He says half of the children who develop severe COVID were previously healthy, and there is no way of predicting which child might suffer dangerous symptoms.
"So from an ethical point of view, you can argue for the direct benefit of children. The universal approach will not only help to protect the at-risk ... but will also help to protect the other half of children who get severe disease or die," he says.
Aside from the primary health benefit, Booy says vaccination provides four secondary benefits: exercise, education, mental health, and socialisation.
Data released by the ANU this week showed young people, particularly teens aged 15 to 18, were suffering the worst mental health effects of the pandemic.
Socialisation with peers is particularly vital to development in that cohort, and Booy says returning to school would lessen the damage of COVID-19.
"I'm keen to see kids get back to school as soon as practical. They are at low risk of disease in any meaningful way; they only get a cold, they don't spread it very easily amongst themselves. [But] teachers should be vaccinated at a very high level," he says.
He says a 70 per cent vaccination rate among teachers and students would be a good starting point, with numbers increasing in line with immunisation levels.
Sanjaya Senanayake, the Hospital in the Home director at Canberra Hospital, argues weekly rapid antigen tests - daily may be impossible - would be a useful added layer of protection around schools.
He says the latest data from NSW reinforces the belief that children are still more likely to contract the virus from an adult than from each other.
Dr Senanayake concedes best practice is difficult to enforce among young children - masks are "uncomfortable, they don't understand [them], and they don't do it properly" - but insists the risk that comes from reopening schools needs to be balanced against the threat of transmission at home.
"I don't think there's any ideal solution. There are pros and cons with whatever model you choose," he says.
"The important thing with COVID is that you just have to adapt. You can't say 'This is what we will do and we will not change.'
"[You have to say] 'We'll see if it works ... but if it doesn't, then we will reassess and adjust accordingly.'"
Dr Senanayake says young children made up roughly one-third of total cases in NSW, but only 5 per cent of hospitalisations. He plays down the prospect of siloing off children into their year groups to reduce transmission.
"Particularly with the younger children, that's going to be really hard to do in practical terms. And the older children should be able to tolerate masks," he says.
Improving weather could make learning outdoors, where the virus is less likely to be transmitted, more feasible, he says. And he adds that open windows in summer will increase ventilation.
MORE COVID-19 NEWS:
But the effects of opening a window in schools have not been analysed in-depth, with studies on ventilation tending to focus on hospitals and healthcare settings.
ANU global environmental health professor Sotiris Vardoulakis says insights can be gleaned from those studies, but warns they are no panacea.
"The difference is the way children move around a classroom environment, which may be different to the way workers ... use a workplace," Professor Vardoulakis says.
"Natural ventilation will help, no doubt. So if we just open the windows, increase the air exchange rates, and have natural ventilation that will reduce the risk of transmission.
"There is [also] some evidence from recent studies that portable air cleaners can also help."
There have been almost 23,000 COVID-19 cases in Australians aged 19 or under, including 10,000 in those younger than 10.
The Delta variant has spread rapidly across the board but, with Australia's older population more highly vaccinated, young people account for a higher portion of cases than in previous outbreaks.
In the US, one of the world's worst-hit countries, 464 people aged under 18 have died from COVID-19, around 0.07 per cent of the overall death toll.
Dr Senanayake says areas with low levels of vaccination in the US are showing much higher infection rates among children.
Areas of low vaccination are also likely to feature less mask wearing and social distancing.
"But another possibility is that the higher levels of vaccination in the adults and adolescents are protecting the younger children to some extent," Dr Senanayake says.
"It's another good indication to think about making sure that everyone who can get vaccinated does get vaccinated."
Nick Coatsworth, an infectious diseases physician at Canberra Health Services, agrees the best protection for children is fully vaccinated adults around them.
He warns even hospitalisation figures for young children can be negatively skewed. On Thursday, ACT authorities confirmed the one child under 12 in hospital was there for "social reasons".
He says young children are often hospitalised with COVID when their parents need treatment.
"Yes, the kid's got COVID, but they don't actually need to be in hospital. They're there because the quickest place you can look after a kid in our society is a hospital if their parents can't look after them," Dr Coatsworth says.
"That distorts and sort of overplays why kids are going into hospital.
"And so the message is then absolutely clear about what we should do: the best way to protect under-12-year-olds is to have both parents vaccinated."
- with Sarah Lansdown
Our coverage of the health and safety aspects of this outbreak of COVID-19 in the ACT and the lockdown is free for anyone to access. However, we depend on subscription revenue to support our journalism. If you are able, please subscribe here. If you are already a subscriber, thank you for your support. You can also sign up for our newsletters for regular updates.
Our journalists work hard to provide local, up-to-date news to the community. This is how you can continue to access our trusted content:
- Bookmark canberratimes.com.au
- Download our app
- Make sure you are signed up for our breaking and regular headlines newsletters
- Follow us on Twitter
- Follow us on Instagram


