When 34-year-old Caitlin Moorhouse experienced a sharp pain in her shoulder, she put it down to lifting her beautiful and much-wanted newborn daughter.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The Griffith public servant, who had always enjoyed good health save for requiring fertility treatment to conceive Violet, was referred for an ultrasound scan on the suspicion it could be referred pain from her gall bladder.

By that afternoon, her doctor had to tell her the unspeakable truth. Her liver was riddled with secondary stage 4 cancers – too many to count.
In what medical experts are now warning is a new frontier in cancer diagnoses among young people, Ms Moorhouse was eventually found to have bowel cancer.
It was advanced and it had invaded her body without any symptoms or family history.
While it is often regarded as an older man's disease, a 2015 report in the Journal of the American Medical Association predicted that by 2030, "the incidence rates for colon and rectal cancers will increase by 90.0 per cent and 124.2 per cent, respectively, for patients 20 to 34 years".
In Australia, the official snapshot is that about 1000 – or 7 per cent – of the 16,000 cases each year are diagnosed in people younger than 50.
But those figures are outdated, and younger people could now represent as many as 15 per cent of cases – a figure in line with the US – according to leading colorectal surgeon Associate Professor Graham Newstead.
Dr Newstead, who heads the colorectal unit at the Prince of Wales Private Hospital, said he and his colleagues were increasingly alarmed by the increased diagnoses among young people.
It was still not understood whether this is the result of environmental factors – such as an increase in processed foods in diets – or genetic predispositions, or a mix of both.
Dr Newstead's unit last year treated two young women in advanced stages of pregnancy who were discovered to have bowel cancer with secondary tumours and that these presented "particularly challenging and heartbreaking cases".
For Ms Moorhouse and her husband David, the months since diagnosis have been a blur.
They have had to uproot to Melbourne to live with Ms Moorhouse's mum while she is under the care of a dedicated team at Peter MacCallum Cancer Centre.
"At diagnosis I specifically asked not to be given a time frame – I knew that being given an estimate of my remaining time would haunt me. Looking back, this was the best decision I could have made," Ms Moorhouse said.
"For my diagnosis, there was a 5 per cent chance of survival over a five-year period. It's now been upgraded to a 20 per cent chance due to better drugs and treatment options. But it was certainly a grim diagnosis to receive."
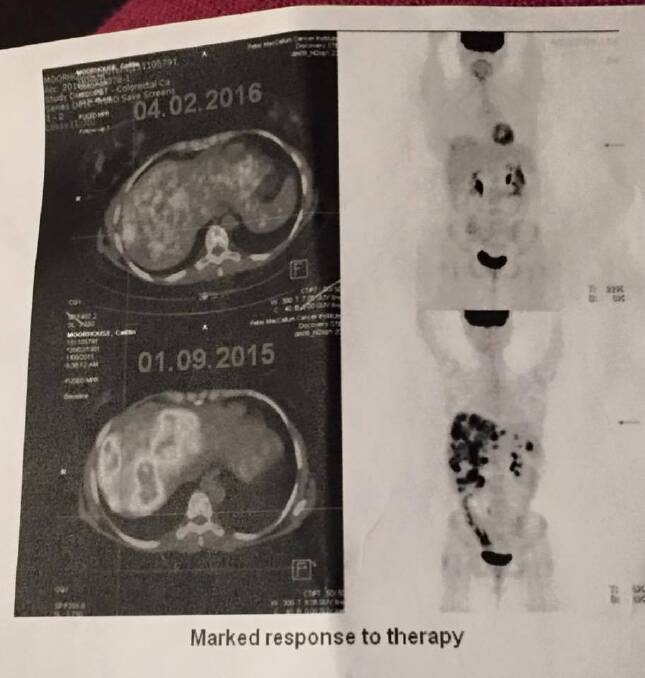
Thankfully, Ms Moorhouse is responding well to treatment. A recent scan showed clear areas where ominous dark patches previously lay.
The race is on to further shrink these tumours enough for surgical intervention. She is holding on tight to the change in wording on her treatment plan from "palliative" to "chronic" and says that after 11 rounds of chemotherapy, she will "likely continue until my body can't take anymore".
All of this, of course, has taken place against the backdrop of caring for a newborn.
But Violet is blessedly an easy baby, and has not seemed to mind the upheaval in her short life – often providing a happy distraction to the other cancer patients sitting with her mother during each chemo session.
"It has certainly added a whole new layer of complexity to parenthood. We have a lot of support from my family and friends but there remains a real challenge in juggling parenting and treatment. Practical things like having to run out the night before treatment to make sure we have enough formula for the week. Or taking Violet to chemotherapy and hoping she doesn't have a meltdown or bother other patients. Or lying in bed too sick to move and hearing your baby crying while the babysitter tries to calm them," Ms Moorhouse said.
Her husband David had been a rock. He combines caring for his wife and daughter while working as an electronics engineer for Seeing Machines, a tech company based in Braddon.
"The diagnosis was a big shock and it's something we'd prefer not to be dealing with. The choice of Peter MacCallum for treatment has proven to be a good one – I have confidence that Caitlin is getting the best care possible. Our oncologist and specialist nurse are both great communicators, and are happy to have robust conversations about Caitlin's treatment options," he said.
Meanwhile, Ms Moorhouse wants more young people to be aware of the facts – that bowel cancer is something they need to know about – both in making lifestyle choices and in seeking screening. And if they have any symptoms at all, they should see their doctor about a referral for a colonoscopy.
Dr Newstead said: "You might be young, with no family history, but please be aware of any change in bowel habit or any blood. Don't assume its haemorrhoids, take steps to disprove it is bowel cancer rather than simply assuming it is not."
Government screening programs recommend a colonoscopy every five years after the age of 50.
There is also a chemist faecal immunochemical test that can be done at home, with Dr Newstead suggesting it may be worthwhile for people in their 40s or 30s to undertake.

