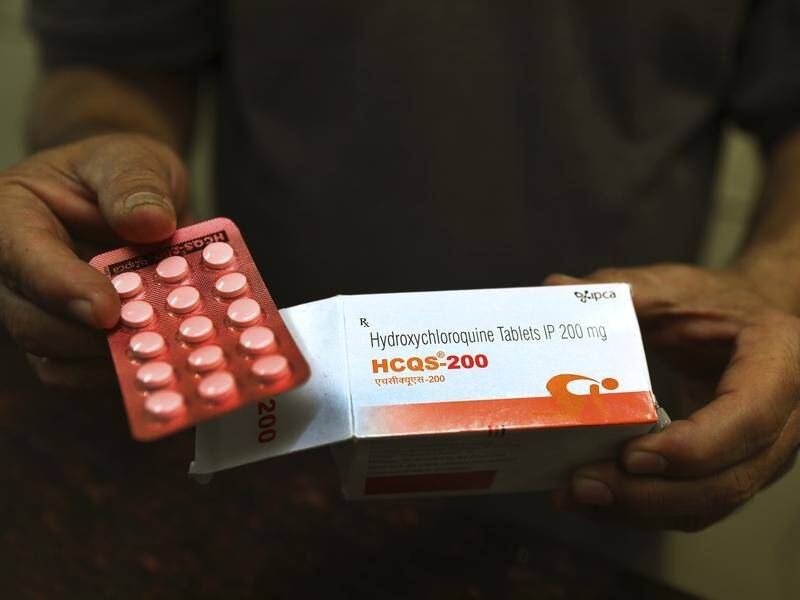
A malaria drug lauded by Donald Trump and a HIV treatment will be trialled on coronavirus patients as part of Australia's first major clinical treatment trial.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Patients infected with the deadly virus at the Royal Melbourne Hospital and Royal Brisbane and Women's Hospital are the first to be screened for the trial, dubbed the AustralaSian COVID-19 Trial (ASCOT).
There are plans to recruit about 2000 patients in more than 70 hospitals across the country, as well as 11 hospitals in New Zealand for the trial, led by Associate Professor Steven Tong from the Royal Melbourne Hospital and Doherty Institute.
It is mainly funded by through philanthropic efforts, including a $1 million donation from mining magnate Andrew Forrest's Minderoo Foundation and a $1 million donation from paper giant Anthony Pratt's the Pratt Foundation.
There is currently no cure for COVID-19 but researchers believe there are multiple treatment options that may be effective.
Laboratory tests have shown that lopinavir/ritonavir, which is currently used to treat HIV, and hydroxychloroquine, used to treat rheumatoid arthritis and malaria, can stop coronavirus precursor SARS-CoV-2 in its tracks.
The World Health Organisation considers both drugs to be promising and has included them in their own worldwide trial, while US President Donald Trump caused a run on hydroxychloroquine earlier this month when he promoted it as a treatment for coronavirus.
More research, however, is needed to be sure they are safe and effective.
"The aim of ASCOT is to test whether using these drugs will prevent patients deteriorating to the point of needing a ventilator in the intensive care unit," Associate Professor Tong said in a statement on Tuesday.
"We have designed the trial so that it's responsive and adaptive. This means that if one of the drugs is proving to be effective, we can adapt the trial to focus on that treatment.
"Conversely, if a drug isn't effective, or is causing severe side effects, we can stop it."
He said having a coordinated approach both nationally and in New Zealand means many patients participate and evidence can be gathered "as quickly as possible".
"Ideally, as other potential treatments become available, these can also be tested within the coordinated framework of ASCOT," Associate Professor Tong said.
Patients will be randomly allocated to different treatments, meaning some will not receive either drug.
"This will allow us to answer whether patients who received a specific drug fare better, worse or the same compared to patients who received a different drug or standard of care," he said.
The trial is expected to run for 12 to 18 months and as the pace of infections slows in both Australia and New Zealand, researchers are approaching other countries including Singapore to join the trial.
Australian Associated Press

