Patients eligible for public dental care are waiting years for treatment.
Subscribe now for unlimited access.
or signup to continue reading
Across Australia, maximum wait times spanned from 1.5 to 3.9 years, according to 2020-2021 data from the Australian Institute of Health and Welfare (AIHW).
"Some people wait a considerable time before receiving care, or an offer of care," the AIHW said.
The Australian Dental Association is tracking delays across Victoria using data obtained through Freedom of Information, offering current wait times for Victorian public dental patients.
Patients in Victoria are waiting more than two years, and up to four years, the longest delays experienced in a decade.
The average wait time for Victorian public dental patients is 26.7 months.
"Our system is only funded to treat a very small proportion of the eligible patients," said Associate Professor Matthew Hopcraft CEO of the Australian Dental Association Victorian Branch.
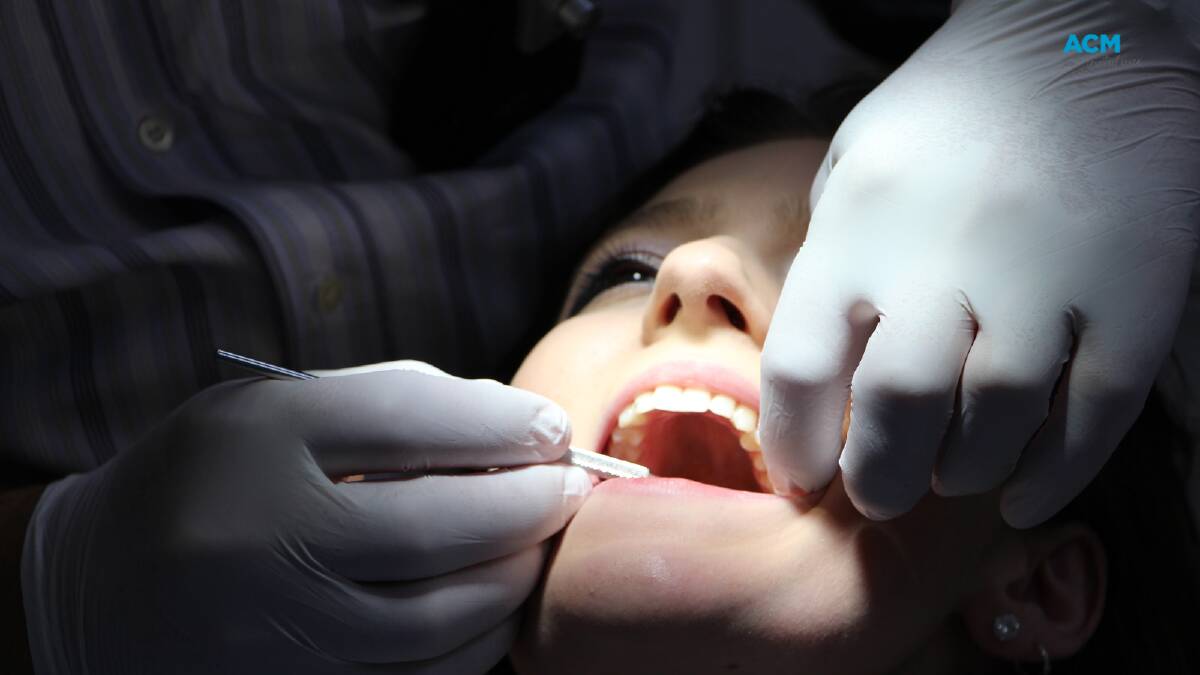
Victoria has 1.5 million patients eligible for public dental health, but only 181,000 received care between June 2021-2022.
Patients with urgent needs are seen more quickly, around 45 per cent of care provided by public dental services in Victoria are emergency procedures, not preventative care.
"The system gets caught in a cycle where they're putting out spot fires," he said.
Head of the Melbourne Dental School Professor Alastair Sloan said delaying dental care could cause an "increased risk of systemic problems".
Infections, left to develop, can kill nerves, cause bone damage and spread bacteria through the bloodstream, Professor Sloan said.
"You don't physically see oral diseases until it's too late," he said.
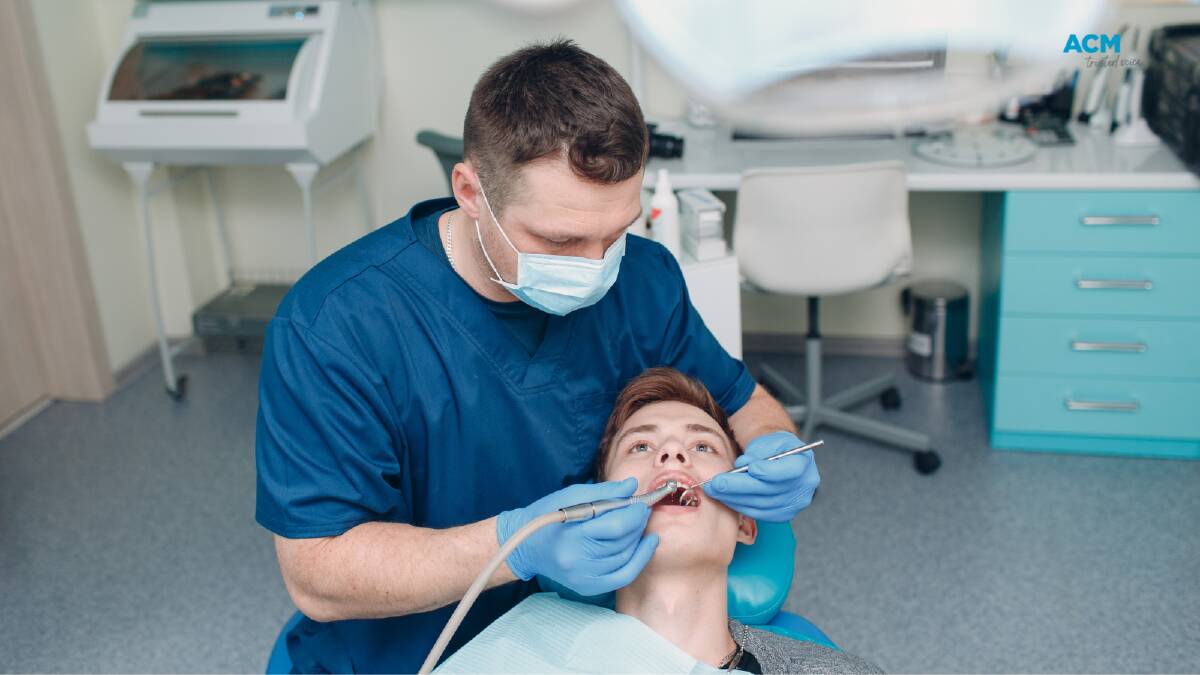
Professor Sloan said long waiting times left patients dealing with mental health symptoms associated with dental disease, including a lack of confidence smiling and talking in business and social settings.
The mental toll of enduring extreme pain over time can be considerable, he said.
"I wouldn't be surprised if we see individuals waiting for treatment with significant mental health problems," Professor Sloan said.
IN OTHER NEWS:
For low-income Australians, the available options for pain management are limited.
Doctors working in general practice will avoid prescribing a long course of analgesic pain relief due to the risks associated with pain medication addiction.
A public health service nurse told ACM that patients presenting to their emergency department with tooth pain were often given clove oil and sent home, despite those patients reporting extreme levels of pain.
Infection is common in patients with oral discomfort, so antibiotic prescriptions are routine for dental patients presenting at GP clinics or hospitals.
This course of treatment can stave off infection but fails to address the root cause of the pain.
"Unnecessary" antibiotic prescriptions contribute to the growing spectre of anti-microbial resistance in Australia and around the globe, Associate Professor Hopcraft said.

"Dental care is not seen as being as important, politically, as other areas of health," Associate Professor Hopcraft said.
Professor Sloan said funding for dental health research was "out of sync" with the disease burden oral health issues carry.
Tooth decay and gum disease are "both infectious diseases and highly preventable", he said.
Associate Professor Hopcraft said these diseases could be minimised in society through education and good oral hygiene, particularly in programs delivered to young children and older adults.


