Nearly one in three women are uncomfortable talking to their general practitioner about having an abortion, while almost one in five are concerned about taking an abortion pill, new research indicates.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
GPs in Canberra will soon be able to prescribe drugs like MS‑2 Step, closing a gap in ACT law that had forced women to go over the border to access lower cost medical abortions.
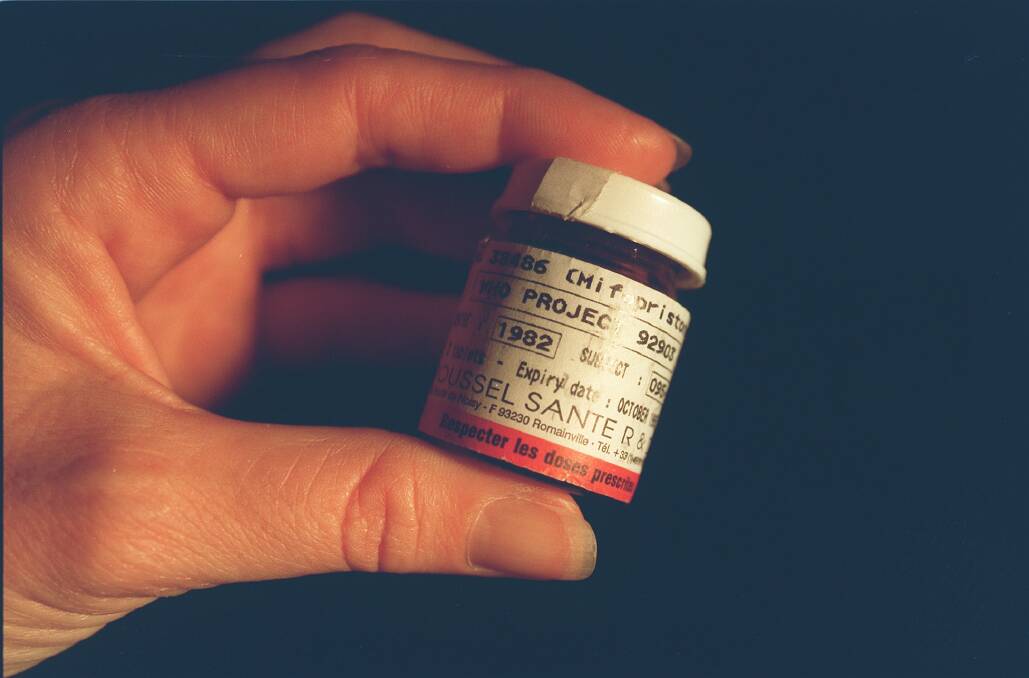
However 30 per cent of women surveyed by The Women's Centre for Health Matters said they wouldn't feel comfortable talking to their regular healthcare provider about an abortion.
Nineteen per cent said they would not feel comfortable taking the medical abortion pill, with one respondent saying they thought it would be "more traumatic and risky".
Women's Centre for Health Matters chief executive Marcia Williams said there was a need to educate both women and health professionals and address some of the "assumptions and myths out there".
"There is a lot of misinformation out there," Ms Williams said.
"Asked that question though, if that [medical termination drugs] was available direct from their GP would they feel comfortable taking it, overwhelmingly 81 percent said they would prefer that."
The centre surveyed 504 women, and held focus groups with 54 women and 24 nurses and doctors on the state of the health system for women in Canberra.
It found cost was the biggest barrier to accessing reproductive services, with nearly one in five respondents saying they had trouble accessing contraception and almost a quarter saying the high cost of a termination would deter them from having an abortion.
It also found the ACT's low bulk-billing rate (57.8 per cent of ACT visits were bulk-billed in in 2016-17 compared to 84.3 per cent nationally) and high number of residents delaying GP visits due to cost (7.1 per cent) had potentially serious consequences.
While 85 per cent of respondents reported having sex in the last year, only 21 per cent said they'd had an STI check in the same period.
Seventeen per cent of respondents said they didn't feel well informed about contraceptives, with most still relying on the male condom (29 per cent) or the oral pill (24 per cent).
Worryingly, 8 per cent relied on the withdrawal method and 4 per cent used other natural methods like fertility-based apps.
Health professionals interviewed for the report described the false advertising of the apps as "dangerous", as it led women to believe they were using an effective method of pregnancy prevention.
"Some of those apps drive me crazy with the advertisement on Facebook for them: 'Doctors have been telling you you need chemicals for contraception for all these years, and here’s this natural free way to make sure that you don’t get pregnant'. It’s like good luck with that. It’s called the Billings method and here’s my children. Like, it’s not a reputable," one health professional said.
Eighteen per cent of those surveyed said they had experienced barriers to contraception, the largest being affordability (34 per cent), time barriers (23 per cent), incompatible contraception (12 per cent), confusing information (12 per cent) and limited services available (6 per cent).
Survey respondents said the combined cost of the appointments and contraceptives, lack of eligibility for subsidised pricing and the lack of bulk-billed services were problems.
“It's ridiculous that I need to pay so much to see a doctor to get the script then to pay for the medication I have taken daily for over 20 years," one woman in the 30-39 age bracket told the researchers.
"Often I put it off as I don't have the time or money to see a doctor. Men don't incur this expense.”
“Without having had a child, women are recommended to be sedated while the IUD is inserted. The cost of anaesthetic and procedure is around $300. While this is cheaper than the pill over the life span of the IUD, this up-front cost may deter many from using the IUD as public waiting lists can be quite lengthy,” another woman in the 19-29 group said.
One health professional interviewed described teenagers risking unplanned pregnancies because of the high cost of emergency contraception.
“The morning after pill is between $30-55. The actual cost of them, the cost price is $4 each. So the mark-up is obscene. If you’ve got a 16-year-old who could avoid the termination scenario with a morning after pill, and decides, no, $55 is too expensive and just decides to wing it for whatever. That happens. I saw so many people leave the pharmacy after realising the cost of it,” they said.
Twenty-three per cent said the $500-plus cost of an abortion in Canberra would deter them from accessing a termination.
Survey respondents who'd had an abortion in the last three years spoke of the difficulty in finding the money to have the procedure.
“I became pregnant after recently ending a long term relationship, I was completing my second year of a four-year apprenticeship, living out of home and nearest family were over three hours drive away. I struggled to get time off from work and save up the required $400 in time. I barely ate and walked over six kilometres to work for four weeks to save the money in time to have the termination before it was too late to proceed,” one woman said.
The report said the ability of GPs to prescribe medical abortion drugs would provide women with "a more accessible and hopefully affordable access to medical abortion".
Ms Williams said the centre wanted to work with the ACT government and the Capital Health Network to help make women's reproductive health services more accessible and affordable across the board.

