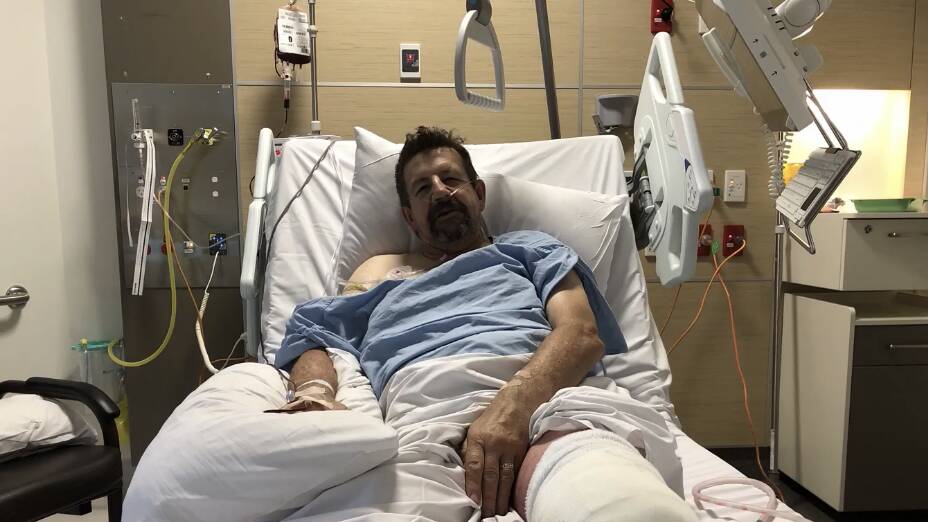
In 2018 I met an everyday Aussie bloke whose story had a powerful impact on me. Neil Hansell constructs light machinery for a living. He has a wife and four kids. He also has type 2 diabetes. A few years ago, diabetes changed Neil's world overnight.
Subscribe now for unlimited access.
or signup to continue reading
Neil is just one of the estimated 1.6 million Aussies living with type 2 diabetes, the sixth biggest killer in our country, a growing epidemic, and the greatest threat to our health system.
Unfortunately, Neil had neglected his health, and he paid the price. He went to sleep one evening with normal eyesight and woke up the next morning blind in both eyes.
One of my surgical colleagues worked hard to retrieve his sight, however sadly, it was too late.
At the age of 50, Neil was faced with the rest of his life in darkness, and all that he can see now are black objects on a grey background.
Neil had to give up coaching the javelin, a hobby and a passion that gave him so much pleasure. He lost his driver's licence, his independence, and his ability to see the beautiful smiles on the faces of his grandkids.
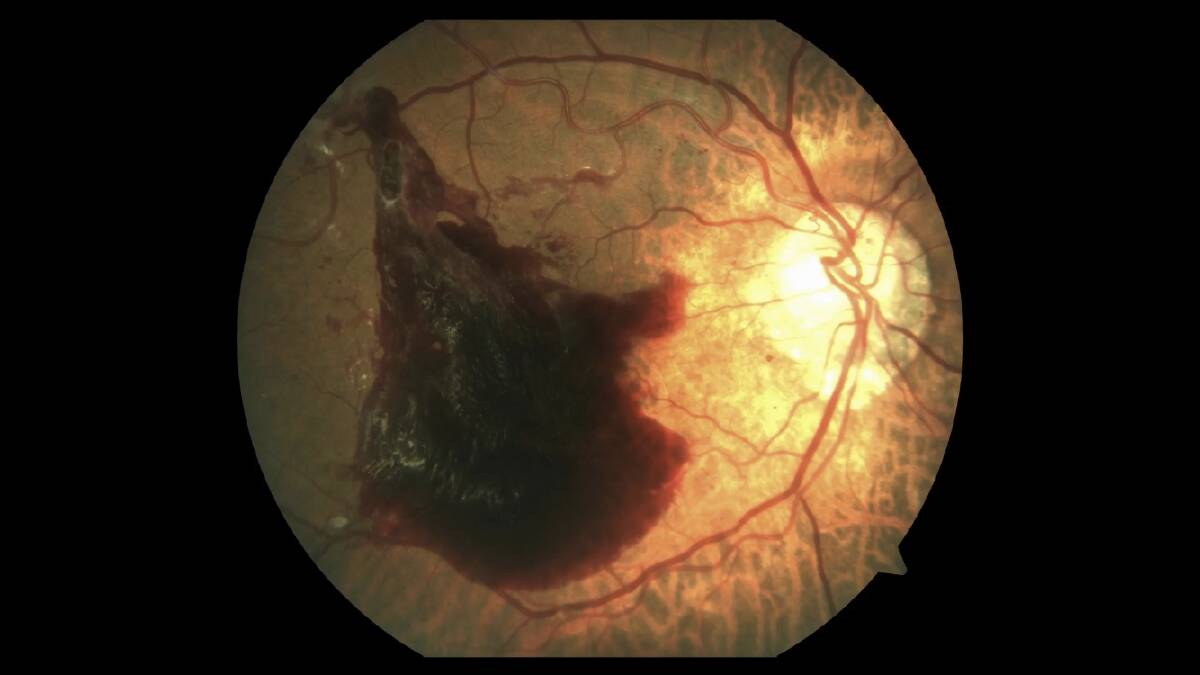
Neil is not alone. Over half of all Aussies with diabetes are not having regular sight-saving eye checks. As a result, it's now the leading cause of blindness among working age adults. It's also the fastest growing cause of blindness in Aboriginal people.
Gangrene of the feet, amputation of the lower limbs, impotence, kidney failure, heart attack and stroke are just some of the other life-changing or life-threatening complications that await people with this insidious disease.
Dealing with the complications of diabetes is expensive. The total annual cost in Australia is estimated to be close to $20 billion.
So, we should all be aware of the risk factors and how we can prevent the disease in the first place, not waiting for complications to arise before we act.
What is diabetes?
The word diabetes comes from the ancient Greek "to pass through" and suggests excessive urination, one of the earliest symptoms of the disease. There are two main categories:
Type 1 diabetes: Making up 10 per cent of all diabetes, it's due to auto-immune damage to the pancreas, the organ that secretes insulin into the bloodstream. Insulin is the hormone responsible for moving dietary glucose from the blood into every cell of our bodies, where it's stored and used as an energy source.
Without insulin, blood glucose levels rise dangerously, and this can be life-threatening. The onset is usually rapid and can happen at any age.
Type 2 diabetes: making up nearly 90 per cent of all diabetes, this is a progressive metabolic disorder where the body becomes resistant to the effects of insulin. Modifiable risk factors include an unhealthy diet (too much added sugar and refined carbohydrate), physical inactivity and weight gain (a gain of 20-35kg increases the risk by 11,300 per cent).
But there is strong evidence we can prevent the development of type 2 diabetes with lifestyle behavioural changes.
Why type 2 diabetes is rising
Humans are physiologically hardwired to love and seek out sweet things. It's an ancient survival mechanism that evolved to prepare our bodies for expected periods of fasting when food supplies were scarce and to warn us off bitter and potentially poisonous foods.
Prior to the 1600s, sugar was an expensive commodity, the domain of healers and holy men or an indulgence for the wealthy and powerful. Its rising availability and popularity over the next three centuries, as a result of the booming sugar trade, led to diminishing costs, turning sugar into an everyday necessity.

These days sugar is cheap and sweet products are everywhere. But things took a turn for the worse in 1980, when American Dietary Guidelines were released in response to the rising incidence of heart disease noted in the decades since World War 2.
Based on little scientific evidence, the guielines recommended reducing dietary fat to less than 30 per cent and increasing consumption of carbohydrates to 60 per cent.
The result: heart disease and type 2 diabetes soared. Globally, there's been a four-fold increase in type 2 diabetes since 1980. And the growth has been even more profound in some countries.
The increasing intake of cheap and highly processed foods, an explosion in the consumption of sugar-sweetened beverages (up 30 per cent in Australia in the decade to 2017) and a more sedentary lifestyle ("the sitting disease") has been catastrophic to our health - and the economies of many nations.
In Australia, and many parts of the world, nearly one in every 10 adults has type 2 diabetes. Half of all adults in the US, and in some parts of Australia, have either diabetes or pre-diabetes.
In Australia, more than 1100 teens and children have type 2 diabetes, a disease previously only seen in mature-aged people. There's even been a case reported in a three-year-old child.
Among the Aboriginal population, diabetes has increased 80-fold since 1980. A diet high in sugar and refined carbohydrates underlies the concerning increase in type 2 diabetes among Aboriginal adults and now teenagers and primary school children.
Sadly, such a dangerous diet is all too common in remote communities, where sweet products are in abundance and fresh and healthy foods are scarce and expensive.
What excess sugar does to you
Simple sugars (monosaccharides) are single molecules, such as glucose and fructose. Complex sugars (polysaccharides) are chains of sugar molecules, as found in table sugar (sucrose), high fructose corn syrup (HFCS), refined flour, white rice and potato. Sucrose and HFCS are made up of short chains of glucose and fructose, in equal amounts, and starch is composed of long chains of glucose. These sugar chains are broken down in the gut and their glucose and fructose are then absorbed into the bloodstream.
As the blood glucose level rises following the ingestion of any sugar, the insulin level temporarily rises to move the glucose into our cells (especially the liver, skeletal muscles and pancreas), where it's used for energy or stored for later use.
With excessive and persistent glucose intake, the cells become "full" and can no longer take in more. The overflow of glucose is ultimately converted into fat by the liver, where it accumulates, and can rapidly give rise to fatty liver. The French delicacy foie gras is fattened goose liver, created by force-feeding them high-starch corn meal. Foie gras is produced in geese in less than two weeks. Humans can develop fatty liver within two months.
Fatty liver can in turn give rise to insulin resistance as more insulin is required to deal with the glucose overflow. More fat is subsequently created by the liver.
Fructose is the sugar that gives sucrose its sweetness. It makes up at least half of all the sugar we ingest, is not recognised as food by the body, has no nutritional value, and is not under hormonal control. Indeed, it suppresses our appetite control system. Fructose is only metabolised by the liver, is immediately converted into fat, and can act directly to cause fatty liver.
The excess fat created by glucose and fructose is exported from the liver as harmful triglyceride and is deposited in and around the abdominal organs as visceral fat, which is far more dangerous than subcutaneous fat. The resulting increase in the waistline is a strong predictor of type 2 diabetes. Indeed, abdominal or visceral obesity is part and parcel of the same disturbed metabolic process.
Type 2 diabetes takes on average 13 years to develop following the onset of insulin resistance. But in children and teens the disease can develop within two years. The diagnosis is often made years after the onset of the disease and it's common for people to have type 2 diabetes for five to seven years before diagnosis. Fatty infiltration of the pancreas impairs insulin production and eventually results in a measurable increase in the blood glucose level.
The ensuing hyperglycaemia (high level of glucose in the blood) leads to the characteristic early symptoms of excessive thirst and urination, and drives continued insulin production. The vicious cycle of metabolic dysfunction progresses, and the sustained hyperinsulinemia (high level of insulin in the blood) is responsible for many of the severe and life-threatening complications of type 2 diabetes.
Persistent hyperinsulinemia and hyperglycaemia will in time damage the fine blood vessels throughout the body, resulting in numbness and pain of the extremities, impotence, kidney failure, blindness, and dementia. Hyperinsulinemia itself predisposes to the development of atheroma (fatty plaques) which can block the major blood vessels, leading to gangrene of the feet and amputation of the lower limbs, heart attack, stroke and death. It also plays a role in causing other diseases such as Alzheimers, hypertension and cancer. Type 2 diabetes truly ravages the entire body.
How to prevent and cure
Naturally occurring dietary fats, such as those found in avocado, nuts, olive oil, eggs, milk, butter and cheese, have never been linked to cardiovascular disease, and low-fat/low-calorie diets have proven to be universally unsuccessful - lowering your caloric intake simply lowers your metabolism.
What's extraordinary, and surprisingly little known, is that minimising your ingestion of sugar, refined carbohydrates, and highly processed products containing these substances, can prevent fatty liver, insulin resistance and type 2 diabetes. It's proven and powerful.

Once a person has been diagnosed with type 2 diabetes, it can be managed successfully in many people without medications or surgery - with dietary modification and increased physical activity.
There's good evidence that dietary modification and regular periods of time restricted eating or short-term fasting (as our ancestors experienced) can help.
There are several approaches to giving up sugar and for fasting, with plenty of books, social media platforms and apps to help (a patient on any medication for type 2 diabetes should only fastwith guidance from a treating doctor).
I do like the analogy of a leaky tap. We don't invent elaborate mechanisms to deal with the overflow of water from a leaking tap, we search for the source of the leak and fix it. In type 2 diabetes, this means finding the root cause - excessive dietary sugar - and fixing that.
Type 2 diabetes is a dietary disease. So, it needs a dietary cure. Sounds simple right? Unfortunately, not. There are other confounding factors that make this a tougher ask and are related to the toxic impact of sugar. I call them the five "A's" of sugar toxicity - addiction, alleviation, accessibility, addition and advertisement.
Five As of sugar toxicity
Addicted: Much of the human race is addicted to sugar, although not many of us realise. Sugar and other sweet products are as addictive as the nicotine in cigarettes. Like nicotine, alcohol and drugs, consumption of sugar activates the reward centre in our brains, resulting in the release of the neurotransmitter dopamine. This in turn makes us want to do it again, as it feels good. It also gives us cravings. And it's the good feelings and the cravings that conspire to make sugar a very difficult habit to kick.
Alleviation: Because sugar makes us feel good, it's often used as solace when we're down or to relieve stress. It gives us an endogenous dopamine hit which counters the cortisol released during anxious times. But the more sugar we ingest, the more we need to make us feel good. It's a vicious cycle that's hard to break and often drives excessive and sustained consumption of sugar.
Accessibility: We are flooded with cheap, highly accessible sugary food and drinks. You can't walk into a service station without being confronted by a wall of confectionery and you can't check out from most supermarkets without being enticed by chocolates and soft drinks, often at discounted prices.
Addition: The world-wide sugar addiction is compounded by the astronomical amount of sugar and other sweeteners added to food and drinks. In the US, 75 per cent of all food and drinks have added sugar.
Advertisement: Our love of sugar is exacerbated by the relentless barrage of marketing messages for sweet products and the lure of fast and convenient foods in our busy lives.
How to cut your intake
It's not impossible to kick the toxic impact of sugar. At the personal level, it's a matter of being aware of our sugar addiction and slowly winding it back.
Going cold turkey from all sugar would be seriously difficult to achieve given the amount of sugar added to our food and drinks.
During my detox, I began with omitting the obvious foodstuffs loaded with sugar - soft drinks, fruit juices, dried fruit, chocolate, candy, ice cream, cakes and sweet biscuits - and avoiding granular sugar itself - no sugar sprinkled on cereal or stirred in tea and coffee (coffee tastes better without sugar!).

Even these simple strategies are likely to cause withdrawal symptoms such as irritability, headache, sluggish thoughts, and fatigue, which often begin on the very first day.
When I detoxed from sugar, it felt like I was trudging through concrete. And the cravings were unpleasant. It was much tougher than a coffee withdrawal. But it lasted for only three days. The occasional paracetamol tablet helped.
Progressing to the next level might include cutting out commercially-produced everyday foodstuffs that contain excessive added sugar, such as jams, condiments and most breakfast cereals, and heavily-processed foods containing refined carbohydrates, such as products made from white flour (white bread, pastries and pasta) and white potatoes (crisps and fries). White rice is also heavily refined and, as such, is pure starch.
I'm no saint when it comes to eating sugar and carbs (my in-laws call me the "Ice Cream Kid"), but I most definitely don't want to contract type 2 diabetes. "Move more and eat less sugar" is a good rule to live by.
It helps to be aware of those times when we're consuming sugar that's linked to a habit, particularly a pleasurable one such as eating a bag of sugary treats at the movies or a block of chocolate in front of the TV. Definitely avoid snacking on sugar or using it as a reward for a job well done.
Why not replace that bowl of sugary treats on the kitchen counter or staff tearoom with a bowl of nuts, or eat an apple instead of drinking a glass of fruit juice (whole fruit contains fructose but it also contains healthy doses of fibre and vitamins)?
It's also important to be aware of those times when we're using sugar to make us feel better or alleviate stress. The brain doesn't care where it gets its feel-good chemicals from, to balance the cortisol permeating our bodies during anxious times.
There are plenty of other options to replace that scoop of ice cream, bar of chocolate or can of soft drink. Going for a walk, run or cycle, listening to your favourite musical playlist, watching a comedy, or doing a good deed, can all make us feel good, through the same internal mechanisms used by sugar, alcohol and drugs.
Time for a sugar tax?
From a public health perspective, it's about accountability for business, industry and government. A multi-disciplinary think tank is needed - one that engages medical doctors, such as endocrinologists and public health physicians, neuroscientists and nutritionists, as well as marketing experts and government.

We need measures that support recovery from addiction, including detoxing from sugar. Making sweet products less obvious and accessible in supermarkets and other retail settings would be a good start. Move them away from check-out counters to reduce those reflex purchases. Vending machines dispensing sugary food and drinks should be removed from government buildings, schools and universities.
A system for clear labelling of the added sugar content of products should be implemented. The current nutritional guidelines on packaging offer no insight into the amount of added sugar contained within. I like the idea of a "traffic light" rating for the level of added sugar, where red equals harmful, orange equals think twice, green equals safe.
In Australia, we have a five-star health rating system, which is voluntary. As such, it's flawed. What manufacturer would voluntarily put a low rating on food it's trying to sell? And a number of unhealthy products are incorrectly rated as healthy. Orange juice, for example, receives five stars, and yet a glass of juice has nearly as much sugar as a glass of cola.
We need to consider a levy on products containing high levels of added sugar. Sugar-sweetened beverages have been linked to type 2 diabetes, and a levy will effectively reduce consumption. It would also help to offset the massive cost to our health system and raise much-needed revenue for awareness initiatives.
The advertising of sugary products should be minimised, as we have done for cigarettes. We should start with bans on ads targeting children on the internet, free-to-air TV and all the other places they see sugary products he perniciously promoted as "normal". Ads promoting such products should also be removed from government facilities and public services such as trams and buses.
Powerful and hard-hitting multi-media awareness strategies are required - just as we have done for cigarettes - to inform the public of the far-reaching health dangers of sugar, the serious complications of type 2 diabetes, and the reassurance that this disease can be prevented and managed without medication.
The sugar industry and the food and beverage industries need to be included in the discussion. But we cannot let commercial interests stop us from acting to prevent type 2 diabetes in the community. It will require resilience and innovation. It's time for Australia to face this challenge and declare war on type 2 diabetes.
- Australian of the Year Dr James Muecke is a clinical senior lecturer in Ophthalmology and Visual Sciences at the University of Adelaide. He is co-founder of Sight For All.
Australian of the Year
You can help find the 2021 Australian of the Year, Senior Australian of the Year (65 years+), Young Australian of the Year (16-30 years) and Australia's Local Hero by nominating a champion in your community.
The awards are nominated by the public, so visit australianoftheyear.org.au to nominate someone you admire who is helping to make Australia better.
Nominations are open until July 31.