My head is being bolted to the table.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
I'm lying flat on my back on the cold glass slab in the radiation oncology department. The immobilisation mask has been placed over my face and it's being bolted down.
OK, so perhaps "bolted" is a tad dramatic. Or maybe not. The mask of plastic mesh is fitted with what might technically be described as fasteners. They are black, they are shaped like bolts, there are nine of them and the sound of each one clamping into place around my head is a jolt to the senses.
So, yes, my head is being bolted to the table. As the final fastener snaps shut, I am locked into the mask and onto the slab.
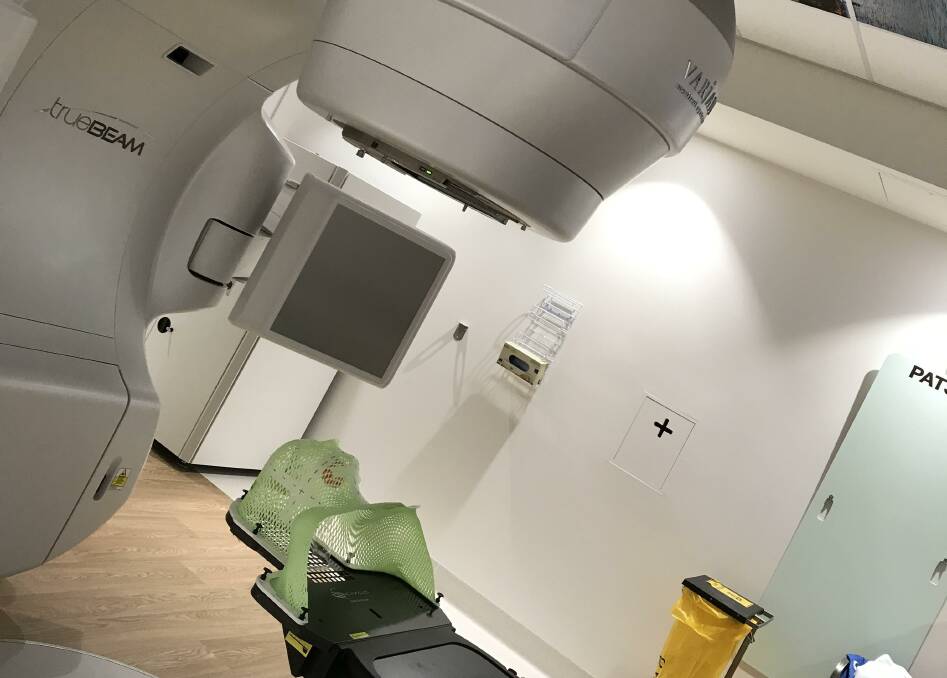
In a few minutes the radiation therapists will ask if I'm OK and then briskly exit what they call the bunker, leaving me alone under the linear accelerator, which will hum and buzz and tilt me on the slab, to aim a beam of high-dose radiation at my head to kill the cancerous cells rampaging through my flesh.
Trapped inside the mask, my heart pounds, my breath quickens and my mind races. Silently, I swallow the desperation.
You cannot freak out about this.
I tell myself not to overthink the situation or the sensations. I stare at the serene lake view on the ceiling above the machine - positioned specifically to give patients something to focus on. Peering through the mesh, the picture is a blur without my glasses.

Then I blink. My eyelashes catch on the inside of the mask. That's how closely it's fitted over my face.
There's another welling of anxiety. I'm trapped. The panic swells like a wave. I can't move. Is this claustrophobia? I can't MOVE!
I catch a glimpse of something freaky in the glass surface of the business end of the linear accelerator as it moves into position to hit me with its little ray of sunshine. It's a reflection of me - the man in the Tupperware mask. The fear surges again, sucking the breath out of me.
Don't freak out. Freak out about the cancer, or the radiation they are shooting into your head. But don't freak out about being trapped in this mask.
Alone in the bunker inside your head inside the radiotherapy immobilisation mask, no one can hear you scream.
Don't panic. Stay still. Breathe.
Weeks earlier I'd been laid out on a different slab, lying still and listening intently as my plastic surgeon sliced a golf ball-sized tumour off the side of my head. There were no waves of panic on his operating table, just the fascinating sound of a scalpel carving delicately at my temple as the local anaesthetic dulled any other sensation.
Now I'm in the radiation oncology department locked into my mask, a beam of high-energy x-rays directed at where the lump used to be, for the first of 36 daily doses of radiation over eight weeks.
What began as an innocuous sun spot has become an aggressive squamous cell carcinoma and despite the plastic surgeon's nifty knife work, by the time the radiotherapy begins the cancer cells are already bulging back through my skin graft.
So, here I am flat on my back and locked in for zapping with a highly charged, carefully calibrated beam of electrons. The immobilisation mask, as the name suggests, is designed to hold my head still and rigid so that ray of concentrated sunshine can target the tumour to the millimetre.
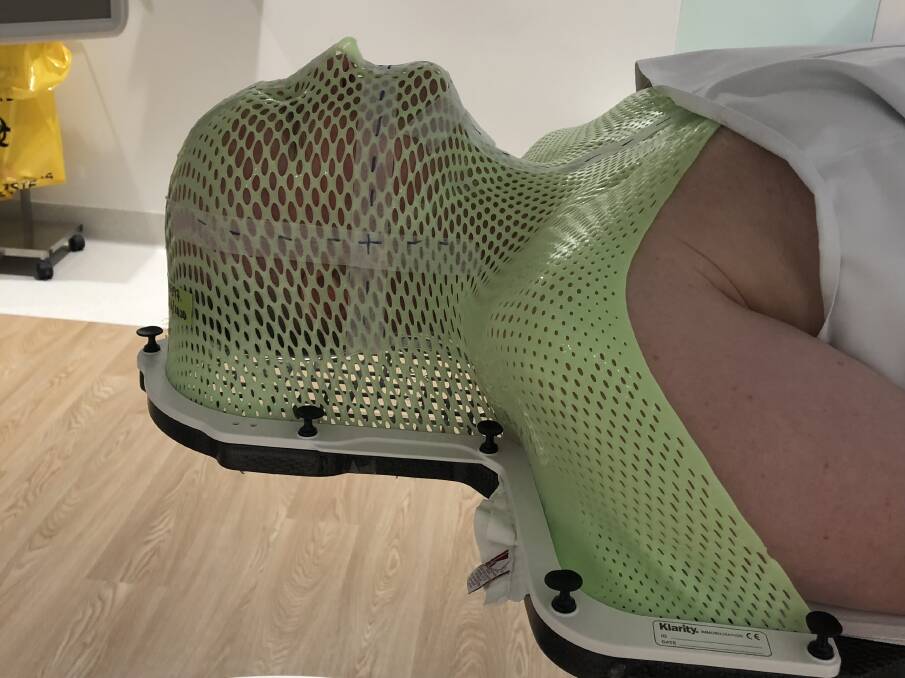
The mask is made of a luminous green polymer mesh and has been moulded to fit tightly to the contours of my face, head and shoulders. I get a preview of what I come to learn is called "mask anxiety" when I am fitted for the contraption days before the treatment begins.
A warm, wet sheet of pliable thermoplastic film is laid over my face and sculpted around my head, nose and neck and shoulders. As it slowly cools and hardens into a me-shaped mould, a brief wave of dread catches me by surprise.
I'm trapped!
The mesh of the mask lets you see and hear and breathe but try telling that to your brain as it races ahead to irrational thoughts.
Don't panic. Stay still. Breathe.
This initial session, called a "simulation", also results in my first tattoos - ink spots on the front centre and sides of my upper torso which will ensure that I am positioned precisely in the path of the radiation. The three black dots will be permanent markers - as are the fearful thoughts that fill my head when I'm bolted down inside the mask.
Feels like being 'buried alive'
An estimated 160,000 Australians are diagnosed with cancer each year, a figure that grows as our population ages. Surgery, chemotherapy and radiation are the main treatments. Radiotherapy is recommended for half of all patients. The Australian Institute of Health and Welfare says the number of radiotherapy courses is rising - up from 61,000 in 2015-16 to 74,000 in 2018-19.
Among those with head and neck cancers, studies show that as many as 50 per cent experience some form of distress in their immobilisation mask.
Yes, "mask anxiety" is a thing, says Dr Jodie Nixon, whose work as an occupational therapist in cancer care led to a PhD on the topic. Her study of patients at Brisbane's Princess Alexandra Hospital showed the levels of stress can be "clinically significant".
"Every person's trigger is so different," she says. "Some say it's a feeling like they are being buried alive." Generations differ too: "A younger, healthier cohort less used to not being in control of their life and choices were more likely to struggle with the mask whereas older patients or those from migrant or lower socio-economic backgrounds were more likely to accept the situation and go with the flow".
Pinned in the mask as the linear accelerator goes to work, it can be a struggle to stay calm as each excruciating minute ticks by. The machine's collimator adjusts the shape, intensity and direction of the radiation beam to match the tumour, but anxious thoughts and palpitations can increase movement and risk damage to healthy tissue, bone or organs surrounding the cancer cells.
"In this day and age you shouldn't have to suck it up," Dr Nixon says. "We should be ensuring care is focused on the needs of the patient." Her study found that relaxation strategies, such as music, visualisation or distraction techniques, and the option to take anti-anxiety medication can help.

So does education before treatment begins. (A Royal Australian and New Zealand College of Radiologists video on immobilisation masks by veteran radio and TV presenter Julie McCrossin, who battled mask anxiety during radiotherapy for throat cancer in 2013, has been viewed more than 25,000 times on YouTube.)
"Time spent up front preparing the patient, explaining the potential impact of the anxiety, is not as costly in terms of efficiency as having to halt the treatment because the patient is having a panic attack," Dr Nixon says. "Simple coping strategies will help those who find the mask unsettling. But those who suffer acute claustrophobia related to previous experiences where the mask is a trigger are less likely to find rainforest music sufficient to manage their reaction."
When I tell Dr Nixon that I declined my radiation therapist's offer to have the radio on while I was zapped (I couldn't risk a random Michael Buble song adding to my torment), she laughs: "Well, if ABBA is more your style, plug in your own Spotify."
Remove the mask
During my treatment, when I post on social media a DIY meme comparing my Halloween-worthy radiotherapy headgear to memorable movie masks, family and friends can't hide their horror.
"I can't think of anything worse than being trapped by the head like that," someone says. "Well, except maybe for cancer," I reply.

Professor Paul Keall leads University of Sydney research devising head and neck cancer radiotherapy without masks but even he admits there is "a spectrum of opinion" about mask anxiety.
"There certainly is a view that you are being treated for cancer so suck it up, that this is a 'first world' problem, that you should just be glad you're getting treated and, jeez, if feeling claustrophobic is the worst thing about your treatment, so what?"
No doubt being bolted to a table would give anyone anxiety but for about half of people having radiation it can go from mildly upsetting to symptoms resembling PTSD.
- Professor Paul Keall
A professor of medical physics and director of the university's ACRF Image X Institute, Professor Keall's "Remove the Mask" project is designing surface-monitoring, cancer-targeting technology that would make immobilisation masks obsolete.
"No doubt being bolted to a table would give anyone anxiety but for about half of people having radiation it can go from mildly upsetting to symptoms resembling PTSD," he says. "Cancer treatments, from surgery to chemotherapy and radiotherapy, can be brutal, so it's telling that so many patients find it terrifying to be bolted down."
Professor Keall's solution is something out of Star Trek. Instead of a mask to hold the patient in position, the radiation beam locks onto the tumour and tracks it even if the patient moves.
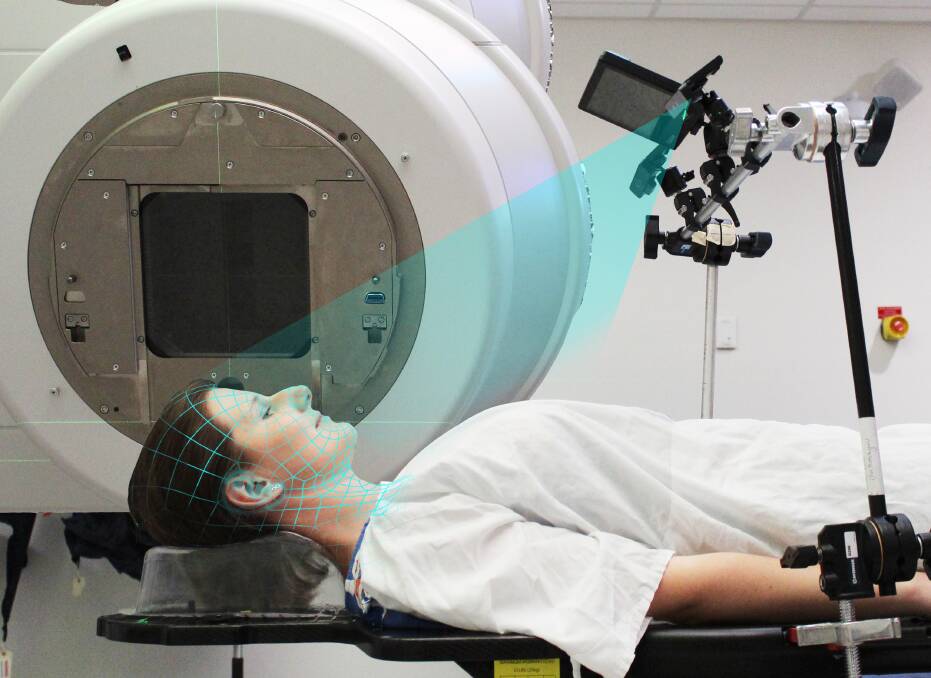
"The mask is there to keep the patient still so in order to remove the mask we need to be able to combine three technologies," he explains. "We need surface-imaging cameras to monitor the patient, x-ray imaging to be able to see the cancer inside the head or neck and we need to be able to adjust the beam to target the cancer so that if the patient moves the targeted beam moves."
The aim is to not only do away with masks, but make radiotherapy more accurate and effective and reduce side effects. "With head and neck cancers there is a very small margin for error because there are a lot of really useful things in that area that help us breathe and swallow and things like carotid arteries and optic nerves," he says.
Drawing on the kind of imaging software used in gaming, Remove the Mask has experiments under way to track "sub-millimetre" patient movements as they lie still. Beam targeting, which ensures the radiation beam "locks on" to the tumour, is already being used to treat prostate and lung cancers.
"For me, the driver is not just removing the mask but asking can we do this treatment better," Professor Keall says. "It's like the evolution of any technology. We now have cars with anti-lock braking and collision-detection and we didn't have those in the past. In Star Trek when you see people in a machine that cures them you don't see them being bolted down under a mask. We are trying to imagine what the future looks like and how we get there."

Clinical trials are a few years away, once technical work and safety checks are completed. He says oncologists and radiation therapists will take a lot of convincing that mask-free radiotherapy is safe: "I don't think many patients would need convincing but patients entrust their care to their doctor and radiation oncologists take that responsibility very seriously so they will need to be convinced about the technology if they are changing a process they trust".
Masking your emotions
Radiation oncologist Dr Purnima Sundaresan, who has consulted on the Remove the Mask project, recognises the need to help head and neck cancer patients "at what is already a quite traumatic time".
"It's exciting to be exploring the possibilities that improved technology might offer," she says. "It's certainly not normal to be confined like that - bolted down so you cannot move - and many people don't recognise they have a problem with the mask until there's that moment of anxiety or a panic attack. But we need to ensure the safety of the treatment because the precision of the radiation is paramount so that all organs at risk around the target area are protected."

In the meantime, health practitioners had to keep the "psychosocial" health of patients in mind. Newly published research by Sydney radiation therapist Melissa Burns, with Westmead Hospital's Dr Sundaresan among the co-authors, shows that while daily interaction through the course of treatment put radiation therapists in the best position to detect and discuss a patient's "situational anxiety", they tend to underestimate the level of distress.
Time pressures, reluctance to adjust efficient work routines and a lack of formal education in identifying and responding to a patient's emotional needs are likely causes. So are patients masking their true emotions.
"Mask anxiety is a type of vulnerability you are experiencing at what is already a very vulnerable time, so many patients are simply trying to control their feelings," Dr Sundaresan says. Men, she adds, are "perhaps less likely, or feel they are less allowed, to talk about their feelings".
Reflecting on my own moments of mute panic under the plastic, I wonder about my grim week in hospital battling an infection after the final dose of radiation. Temperatures raging into the 40s fuelled mind-bendingly macabre, scream-worthy fever dreams - most featuring the luminous green, ghost-like shell of a faceless man.

While many patients never want to see their immobilisation mask again after their treatment ends, and others decorate it as therapy, I souvenired mine. It hangs in my study, watching over my shoulder as I write this. To face my fears, I simply turn my head.
It sounds trite, but two things ultimately helped me ride those waves of torment inside the mask: remembering to breathe, and not forgetting to laugh.
Laughing with my wife when she forbids me from cutting my eyelashes to stop them catching in the mesh of the mask. Instead, she offers me an eyelash curler.
The dark humour of the colleague who dubs radiotherapy the "barbecue roll" - because, yes, being tilted on the slab under the linear accelerator's x-ray beam does sound a bit like how the Apollo spacecraft rotated to protect them from being cooked on one side by the sun.
The generous laughter of my excellent radiation therapists as I'd invite them each day to pop me into my Tupperware container and chuck me in the microwave. Plus their cheeky promise that my mask will always win Halloween. Scary, but true.
- ACM executive editor James Joyce has been cancer free for two years, and has his skin checked regularly as Cancer Council guidelines recommend.

