In the moment before a tsunami strikes land, a strange phenomenon occurs.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Rather than rush forward, water rapidly recedes from the shoreline, exposing the beach or ocean floor underneath.
The so-called "drawback" is the calm before the disaster.
'We would not be immune to this'
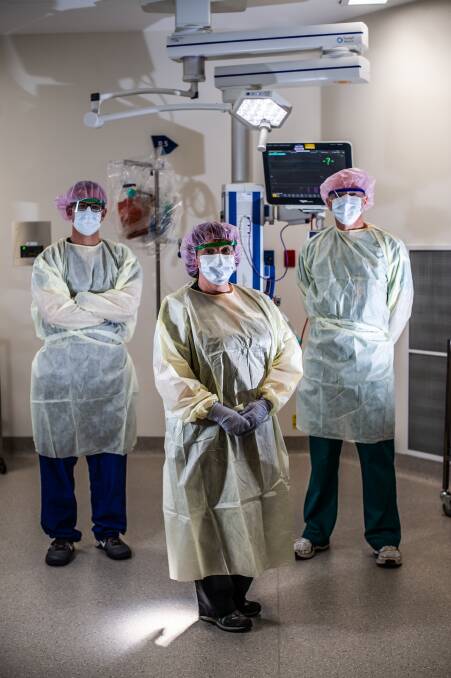
Canberra Hospital emergency department physician James Falconer uses the tsunami as an analogy to describe his greatest fear about the COVID-19 pandemic.
Dr Falconer, like his colleagues, has seen tsunamis form and crash through parts of Italy and New York, with waves of coronavirus patients overwhelming hospitals.
"You can't just look at Italy and say that their health system is rubbish. It's not, they have a very good health system and they've just been overwhelmed," he said.
"We would not be immune to this, we would be overwhelmed as well."
He desperately hopes the tsunami never hits Canberra.
There are positive signs that one won't; that the mix of tactics to suppress the virus' spread, including border closures and tough physical distancing restrictions, have set Australia on a path to avoiding the horrors experienced in parts of Asia, North America and Europe.
But Dr Falconer, together with his colleagues and the ACT government, is preparing for the worst.
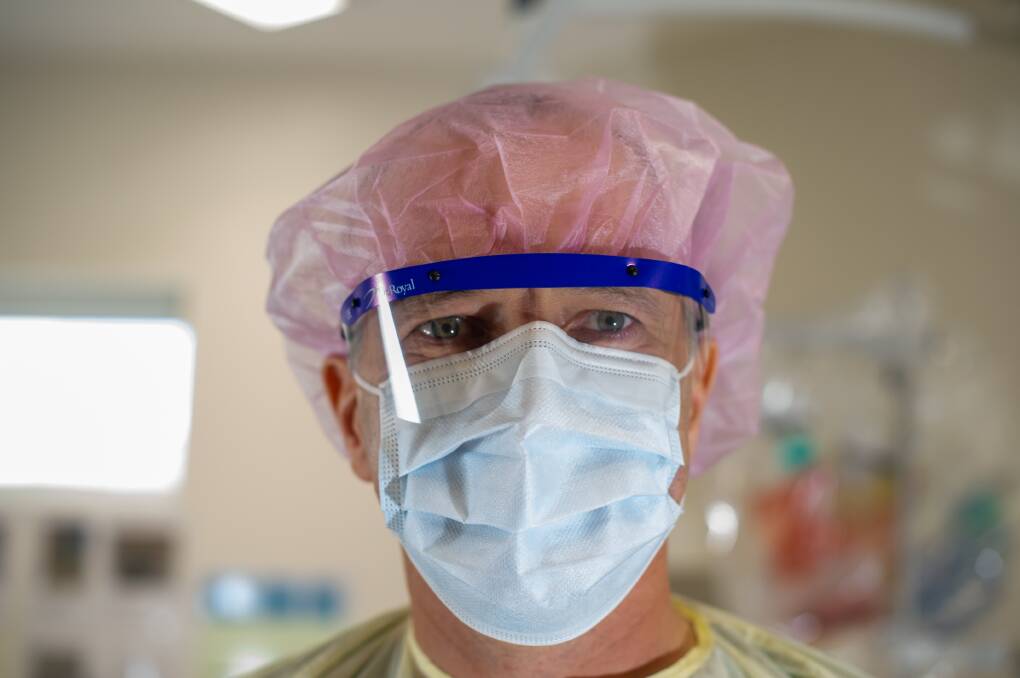
"My fervent hope in six month's time is the media looks at us and thinks you guys were nuts and you massively overprepared and overcalled it and you're paranoid," Dr Falconer said.
"If we are getting to that level we are achieving what we need to do.
"Better to be overprepared than underprepared."
In the coming weeks, Dr Falconer will be among the hospital and healthcare workers sharing their experiences of being at the coalface of Canberra's fight against coronavirus.
Canberra Health Services will broadcast short video diaries from various frontline staff, who will share insights into their daily duties, provide updates on the preparations and send messages to Canberrans.
The Canberra Times last week spoke with a selection of those staff, including doctors, nurses and clinical educators.
Each plays a different role in the fight. Each has a different background, professional experience and perspective.
But they share a common sense of fear and anxiety about the virus; about what it can, and has done, to people, including health workers, around the globe.
And they have a common message for Canberrans, whom they view as essential allies in the battle against COVID-19.
Please stay at home. Please stay apart. Please wash your hands.
"You can make a difference," Dr Falconer said.
"You can maybe save a life. That life might be yours, but it also might be your parent, your uncle, your brother, your sister and your child.
"I am the ambulance at the bottom of the cliff. I do not want people falling off the cliff."
'A sense of fear'
Kate Dwyer, a clinical nurse educator at Canberra's Walk-In Centre clinics, has already experienced a tsunami of sorts - even before the first positive case was recorded in the ACT.

In the days immediately after the Weston Creek Walk-in centre started testing for COVID-19 in early March, the clinic was "overwhelmed" with people desperate to find out whether or not they were infected.
"They were coming [to the Walk-in centre] out of a sense of fear. Anybody who had the slightest runny nose were really just stressed and thinking that the only thing that was going to save them was to be tested," she said.
"That was hard because we needed to follow the strict (testing) criteria and people were getting distressed ... but I can understand their sense of fear."
The ACT government has since expanded the testing criteria, but has also opened up a drive-through testing clinic at Exhibition Park which has helped to ease the burden on the walk-in clinic.
More than 6200 tests have been conducted in the ACT as of Monday, April 13. There have been 103 confirmed cases, more than two-thirds of which have now recovered.
After those frenzied first few days, Ms Dwyer said some anxiety in the community appeared to have diminished as the number of new cases in the ACT and across Australia continued to decline.
"I think people are feeling comfortable that we haven't been climbing at a dramatic rate [of new cases] every day," she said.
But despite the positive signs in recent days, there is still no end in sight to the pandemic. The uncertainty is what makes this event different to anything she has experienced in her career.
"We usually go through trauma and then we are in the recovery phase," she said.
"This is very different in that we are continually in the crisis stage and we are just building and building and building."
'It has taken over my life'
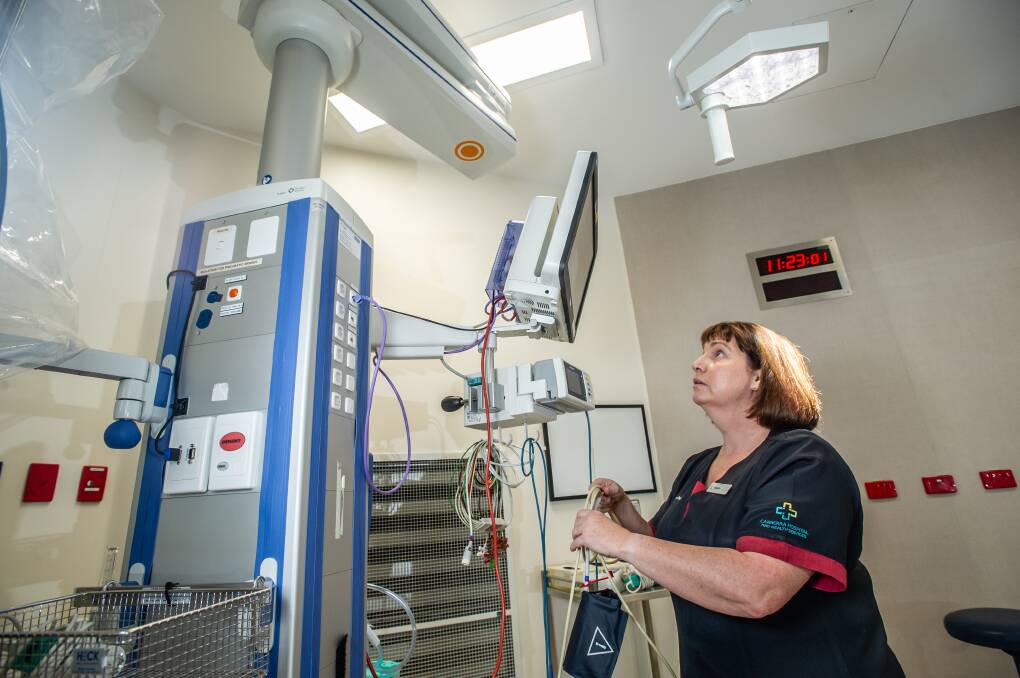
Angela Abigail developed an interest in disaster medicine early in her nursing career. She was part of a team which trained in 2015 to be deployed overseas amid the Ebola outbreak.
But she has never got the chance to put those skills into practice - until now.
"It's quite interesting because we see these things happening overseas in bigger populations and I think sometimes in Australia were are a little bit protected and a bit isolated," she said.
"So to have this stuff on our doorstep is a really unique opportunity for us."
Working as a clinical nurse consultant in Canberra Hospital's emergency department, she said coronavirus had "basically taken over her life". Amid the pandemic, her team has been forced to rethink how they deal with patients when they present to the emergency department.
Now, if someone presents to the emergency department with flu-like symptoms they are immediately isolated from other patients.
"What we have chosen to do is treat everyone like they do have it [coronavirus] until it is proven otherwise. That way we aren't going to miss anyone," she said.
A designated area for staff to change into their PPE (personal protective equipment) has also been set up.
Ms Abigail said presentations to the emergency department had been down in recent weeks, giving clinical staff extra opportunities to run through scenarios which they might confront in the coming months.
"In the first couple of weeks, things changed fairly rapidly. But they have settled in the past week and a half," she said.
"People working here are concerned that we may become infected, but being able to have this time to really upskill and step through the processes has actually really helped build confidence in people that they are going to be OK.
"As a department of 500 plus staff - nursing, medical, clerical and wardsman - it is amazing how much people have really pulled together."
READ MORE:
'We need you to help us'

When a patient's condition worsens and they require more urgent care, Clare Robertson and her colleagues in the intensive care unit are on hand to treat them.
Intensive care patients are monitored around the clock by one or two specially-trained nurses.
A small proportion of Canberra's COVID-19 patients have been treated in the hospital's ICU after becoming infected. Two people have died in the ACT after contracting coronavirus, although neither were in intensive care when they passed.
Those working in critical care are well accustomed to trauma, but that doesn't necessarily mean they are immune to emotional distress.
"No matter how many deaths you deal with, it can still be a very horrible experience," said Ms Robertson, who is a clinical nurse educator in the intensive care unit.
"We do create those professional relationships and you do tend to get to know the families.
"But we are really good at working with the team and we have each other's back. We are really really good at supporting each other and having that sort of community spirit that we are in this together."
When health professionals such as Dr Falconer warn of the coronavirus "tsunami", they are most acutely concerned about patient numbers far exceeding an intensive care unit's capacity.
Health authorities' goal of slowing the virus' spread - of "flattening the curve" - is fundamentally about reducing the number of people who require hospital treatment at any one time.
If Canberrans flout physical distancing rules, they increase the risk of the virus spreading and, in turn, swamping the intensive care units.
That is a scenario that neither Ms Robertson, nor any her colleagues, want to see realised.
"I would 100 per cent tell people to make sure that they stay home and follow the rules," she said.
"We [health professionals] are doing the right thing and staying at home and isolating ourself.
"If you do go out or go to the coast you are just going to spread the virus more and that is going to create a huge burden on the healthcare system.
"Our community needs you to do this for us so that we don't have that huge burden."
- For information on COVID-19, please go to the ACT Health website or the federal Health Department's website.
- You can also call the Coronavirus Health Information Line on 1800 020 080
- If you have serious symptoms, such as difficulty breathing, call Triple Zero (000)
Our COVID-19 news articles relating to public health and safety are free for anyone to access. However, we depend on subscription revenue to support our journalism. If you are able, please subscribe here. If you are already a subscriber, thank you for your support. If you're looking to stay up to date on COVID-19, you can also sign up for our twice-daily digest here.


